Juan Manuel Bellón and Gemma Pascual, Scientific Director and Coordinator of Unit 17 of NANBIOSIS, have recently published an article in the prestigious journal Tissue Eng Part C Methods.
Once a prosthetic material is implanted, an inflammatory reaction is induced in an attempt to remove it or isolate it from the host tissue. After this initial response, a cellular response takes place that gives rise to the start of the process of integration of the biomaterial within the host tissue. Immunohistochemical studies can provide information on the events that regulate this process, and are useful to analyze the progression of the implant and the neoformed tissue. For the tissue repair of a damaged area constantly subjected to tensile forces such as the abdominal wall, optimal collagenization is an extremely important factor. The proper deposition and organization of mainly collagen type I in the neoformed scar tissue will condition the mechanical strength and compliance of the repair zone and thus possible hernia recurrence. In this report, we review the use of the New Zealand White rabbit as the experimental animal for several models of abdominal wall repair and among other techniques, collagen component of the implants was assessed by immunofluorescence using anti-collagen type I and type III monoclonal antibodies. Samples were examined using a confocal microscope Leica SP5 belonging to the platform ICTS ‘NANBIOSIS’ U17 of the CIBER-BBN at the University of Alcalá.
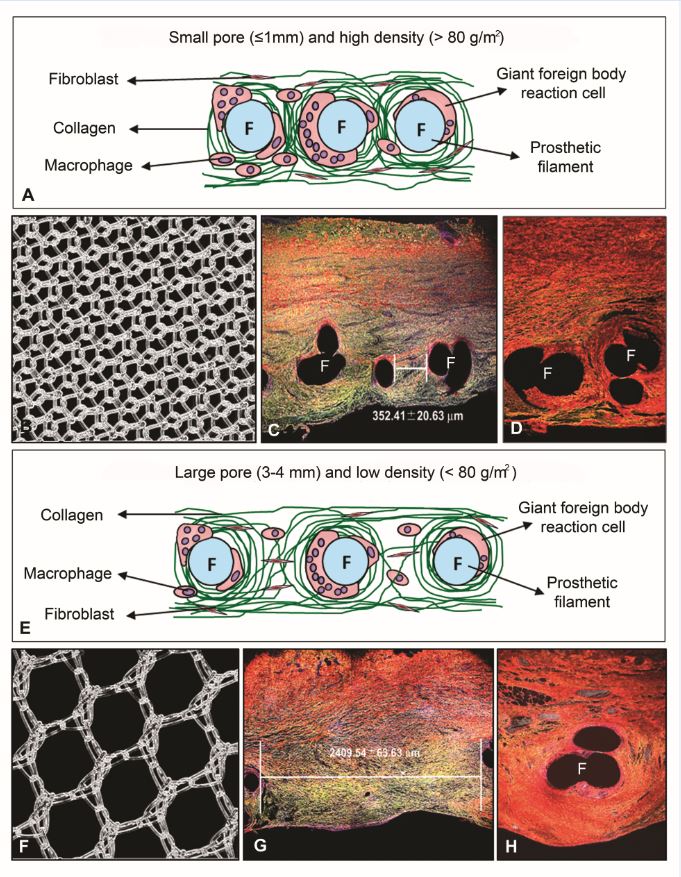
Important information gained from selected models was observed in terms of tissue ingrowth and collagen deposition in the implant area showing significant differences depending on the properties of the implanted prosthetic material. Some variations were also observed in biomechanical properties according to the components comprising each prosthetic material.








